The government must do some heavy lifting on obesity
More than 2.1 billion people -- nearly 30 per cent of the global population -- are overweight or obese. Obesity levels now dwarf the number of people undernourished -- by a factor of almost two and a half times – and account for around 5 per cent of all deaths worldwide.
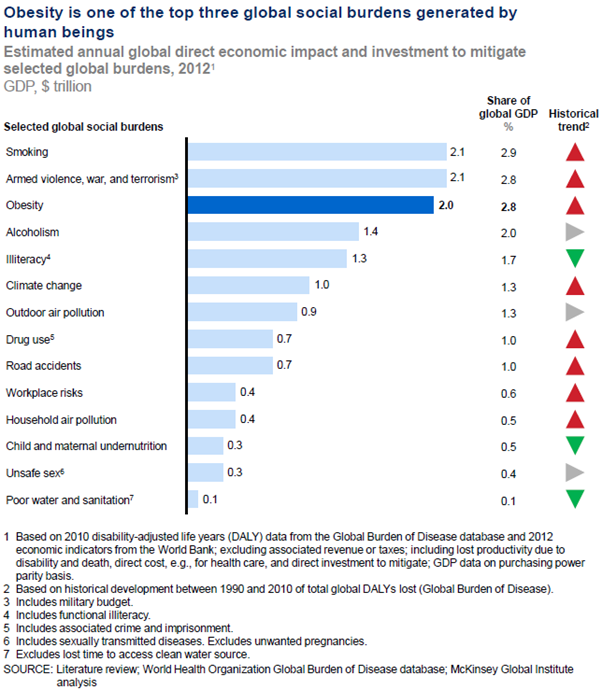
A new report by the McKinsey Global Institute (MGI) turns the spotlight on the economic and social cost of obesity. According to the report, it's one of the top three social burdens generated by humans -- almost exceeding the global cost from smoking and armed violence.
The root cause behind rising obesity levels is many and varied, encompassing evolutionary, biological, psychological, sociological, economic and institutional factors.
According to MGI, “because of centuries of food insecurity, human beings have evolved with a biological ability to cope with food scarcity rather than abundance.”
Biologically humans appear to be poorly designed to deal with periods of food abundance. The effects of this have only been compounded by our increasing sedentary lifestyle; modern life places fewer physical demands on many people.
Psychologically many people have a relationship with food that goes beyond the need for basis sustenance. This can manifest itself in various conditions such as stress eating or addiction to sweets or soft drinks.
Research shows that we are also affected by social norms. According to the report, “one study has shown that 35 per cent more calories are consumed when having dinner with a friend than when eating alone.” We are also 57 per cent more likely to become obese if a good friend has become obese, which highlights the social normalisation of the issue.
Finally, and of particular relevance to developed countries, food is now more affordable than it has ever been. In Australia, spending on food has fallen from 20 per cent of disposable income in 1960 to 14 per cent in 2014. There's a similar pattern in other developed countries, reflecting the growing affluence over the second half of the 20th century.
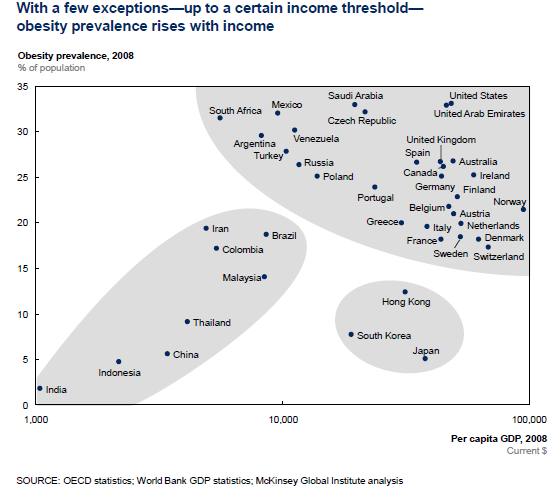
Obesity rates appear to rise with income up until a certain level and then the relationship breaks down. What's more striking, however, is how few wealthy countries manage to break the obesity trap.
MGI estimate that the global economic impact of obesity is roughly $2 trillion, or 2.8 per cent of global GDP. These estimates include the cost of lost productivity through the loss of productive life years, direct costs to health-care systems and the investment required to mitigate the impact of obesity. Lost productivity accounts for nearly 70 per cent of that estimate.
It is also worth noting that these estimates are valued at a cost rather than net present value basis. Problems such as obesity and climate change have costs that are likely to be much higher in the future than they are today.
The most important question though is what can we do to reverse these trends? Surely we don't want to gorge ourselves to death.
The MGI report identifies 74 interventions to address obesity across 18 separate areas. These include portion control, restrictions on advertising high calorie food and drinks, greater education for parents and public health campaigns (the recommendations are contained on page 9 of the report).
No single intervention is a silver bullet; mitigating the economic cost of obesity requires a comprehensive, systemic program of interventions that address obesity from a number of angles.
Using the United Kingdom as a case study, based on an assessment of the economic impact of 44 of the recommendations, the MGI report notes that “if the United Kingdom were to deploy all the interventions … the research finds that it could reverse rising obesity and bring about 20 per cent of overweight and obese individuals … back into the normal weight category within five to ten years.”
Furthermore, almost all of the recommended interventions are cost effective, with economic benefits that outweigh the cost of intervention. These are interventions that offer considerable bang for their buck.
The need for widespread reform though makes it more difficult to gain consensus and coordination between governments, employers, educators, food retailers and restaurants. Realistically there is a significant incentive to free-ride and leave the heavy lifting to other groups; furthermore, it's not clear that all stakeholders would benefit from these reforms.
Obesity is clearly an international problem but it's one that hits close to home in Australia. Australia has the fifth-highest rate of obesity among OECD countries and the share of our population who are considered obese is rising at a rapid rate.
This is the very definition of preventable health crisis and, if the MGI analysis is accepted at face value, significant and cost-effective improvements can be made. Preventable health care took a back seat at the May federal budget -- the National Preventative Health Agency was abolished -- but with health care costs rising rapidly, this is one area in which the government can get on the front foot and save future generations billions of dollars in unnecessary health costs.
















